If your gynecologist has turned down your request for an IUD in the past, it might be time for another try — or another doctor. Older rules said that women who had never given birth shouldn’t get IUDs. That changed years ago, and docs are slowly getting the memo.
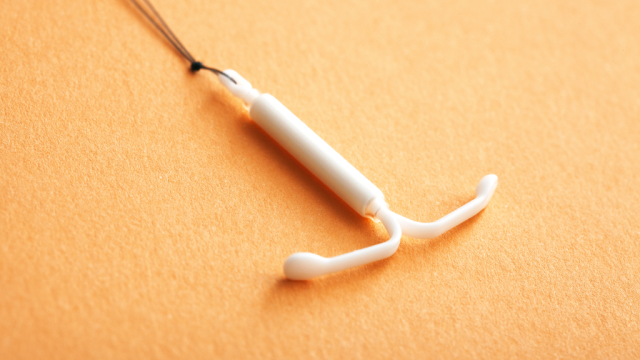
Photo by Image Point Fr via Shutterstock.
An intrauterine device, or IUD, is a nearly foolproof method of preventing pregnancy, and it’s an excellent choice for many women. Even the American Academy of Pediatrics says it should be a first-line option for teenagers who want contraception.
Unfortunately, old ideas die hard. In a 2014 survey of members of the American College of Obstetricians and Gynecologists, 96 per cent said they provide IUDs, but only 67 per cent say that they consider IUDs appropriate for “nulliparous” women (those who have not given birth). Worse, only 43 per cent were willing to give them to teenagers. This is still an improvement from previous years: in 2002, only 32 per cent said they don’t rule out nulliparous women (and only 80 per cent inserted IUDs at all).
Why Doctors Used to Say No
In the early 1970s, an IUD called the Dalkon Shield caused severe and sometimes fatal infections in some women who used it. Over 100,000 women in Australia were fitted with the device, and it continued to be used into the 1980s, even after it had been withdrawn from the US market. Today’s IUDs use a different, safer design, and all medical devices now have to be TGA-approved before they can be sold. That means the Dalkon Shield is a tragic but closed chapter in reproductive health history, not a cautionary tale with relevance today.
The Dalkon Shield left women, and their providers, skittish about IUDs in general, and it’s taken time for that stigma to wear off. Because of that, many doctors weighed risks too heavily against benefits, even as research came out saying that IUDs are safe for most women.
The IUDs’ makers were also cautious at first. Back in 1988 in the US, the Paragard copper IUD’s package insert included a “recommended patient profile” that said the ideal patients are women who have had at least one child, and are in a stable monogamous relationship. The Mirena hormonal IUD was introduced in 2000, and said the same thing.
You Have Better Options Today
Women in Australia have their choice of either a copper or a hormonal IUD, whether they have had children before or not:
- Copper IUDs last five or ten years, depending upon the model you get. It is inserted by a specially-trained doctor and is not covered by the PBS, so it will cost about $150.
- Mirena is the only hormone-releasing IUD available in Australia, and can be prescribed to and inserted in all women by a specially-trained doctor. It is covered by the PBS and will run you around $35, and lasts around five years.
As with any medical device, there may be legitimate reasons why an IUD is not right for you. Gynecologist Jen Gunter summarises the main issues:
- Women with Wilson’s disease (a disorder of copper metabolism) can’t have a copper IUD, but they can have a Mirena
- Women with a progesterone sensitive breast cancer can’t get the Mirena IUD, but they can have a copper IUD
- Women who have fibroids distorting the inside of the uterus or a uterine septum typically can’t get an IUD (this is a fit issue)
- Women who have a uterus that is too small or too big for an IUD (you find out this when the doctor or nurse practitioner checks the uterus right before insertion) also can’t get one. In my experience this is pretty uncommon, maybe 1% of the time.
There’s also, anecdotally, a difference in how women experience insertion. If you’ve never had children, the opening in your cervix is small and insertion may be painful — some say extremely so. For women who’ve already had kids, insertion usually isn’t painful at all, or only mildly.
No doctor today should be refusing you an IUD based just on whether or not you’ve had kids. If they do, call around (or ask a friend where she got hers) because IUD-friendly docs are out there, and they are the majority.
Comments
One response to “If Your Doctor Won’t Give You An IUD Because You Haven’t Had Kids, You Need A New Doctor”
FYI Author, no doctor is obligated to perform any non-life saving procedure on any patient. They have every legal right to refuse to perform anything, prescribe anything, or examine anything, so long as they don’t obstruct your ability to get it from someone else.
Now, there are very good reasons why a lot of doctors won’t offer to insert IUDs for nulliparous women, and you even listed an important one in your article….
“If you’ve never had children, the opening in your cervix is small and insertion may be painful — some say extremely so. For women who’ve already had kids, insertion usually isn’t painful at all, or only mildly.”
So yes, if you really want it you should get another doctor, but to say that the doctors just aren’t getting the memo when they do not wish to perform a procedure that is unnecessarily difficult and painful when there are plenty of easier options that are also very effective, is just silly.
The pain that can be experienced by some women (not all) is also not anecdotal, its studied http://www.ncbi.nlm.nih.gov/pubmed/17531622 many http://www.ncbi.nlm.nih.gov/pubmed/7389354 times. http://jfprhc.bmj.com/content/early/2015/04/08/jfprhc-2014-101046.full (that one is fun, 76% say moderate to severe pain and 46% having vasovagals!)
While doctors are not obligated to provide non-lifesaving procedures, I would argue that they are obliged to provide the patient with accurate and evidence-based information as to why they do not wish to perform the procedure, so as to not indirectly mislead the patient about the efficacy or safety of the treatment.
In my own personal experience, a doctor stated that she would never do an IUD insertion for a nulliparous woman such as myself as it is “always incredibly painful” and puts the patient at “greatly increased risk” of PID – that was the end of the discussion. There was absolutely no weighing up of the risks and benefits, which accompany most all medical procedures.
This has also been the experience of many of my peers. This is not an example of evidence based, patient-minded medicine, and left me, and undoubtedly others, inaccurate information with which to make health-related decisions. It also, arguably, put us at a greater risk of unwanted pregnancy by hindering access to one of the most effective, long-term, and easy to use (after insertion) forms of contraception available.
Some doctors obviously aren’t getting the memo.
I have aural migraines.
implanon made my bipolar play up.
the fact that depo can not be removed, and my reaction to the implanon makes the depo too risky.
Imagine if I went to a doctor who refused to the mirena because of their *personal* opinion?
their personal opinion would mean that I wouldn’t have any birth control.
Imagine now, if I went to a doctor who told me the risks, and then allowed me to make the best choice for my body?